Revision arthroplasty is a procedure performed when a worn-out hip, knee, shoulder, or elbow joint replacement component requires replacement with a new prosthesis. Hip and knee arthroplasties are some of the most common procedures undertaken today. It is estimated that in 10 years, the number of primary total hip arthroplasty interventions will grow by 71% to 635,000 procedures, and primary total knee arthroplasties will undergo an 85% increase, totaling 1.26 million procedures in the United States. Consequently, total hip and total knee revisions are projected to grow by 137% and 601%, respectively, between 2005 and 2030.[1] Shoulder arthroplasty is also a prevalent joint replacement surgery, being the third most common after hip and knee replacement. In terms of complications, total elbow arthroplasty has complication rates higher than that of total joint arthroplasty of all other joints.
The complications associated with a replacement surgery are based on the existing wear and tear of the primary joint and, consequently, the anatomical challenges posed at the surgical site. Surgically, once the failed joint components, cement, and weak bone have been removed, a gaping hole confronts the surgeon. Problems of stability, mobility, fixation, and the reconstruction of bone defects as well as restoration of an anatomic joint require simultaneous attention.
The goal is to establish a properly functioning implant, which depends on appropriate fixation to the bone. This fixation can either be achieved by cementing the implant onto the bone or by using biologic (non-cemented) fixation. The method used for fixation is up to the surgeon and depends on the case.
A revision procedure for a prosthesis that was fixed using cement poses its own challenges. For example, cement removal during hip or knee arthroplasty revision surgery is technically demanding and prone to severe complications such as periprosthetic fractures, incomplete cement removal, or perforations. Several alternative techniques have been developed to enable complete, accurate, and safe removal of cement from bone, including osteotomies and cortical windows, endoscopic instruments, ultrasound devices, lithotripsy, and laser-assisted removal.[1]
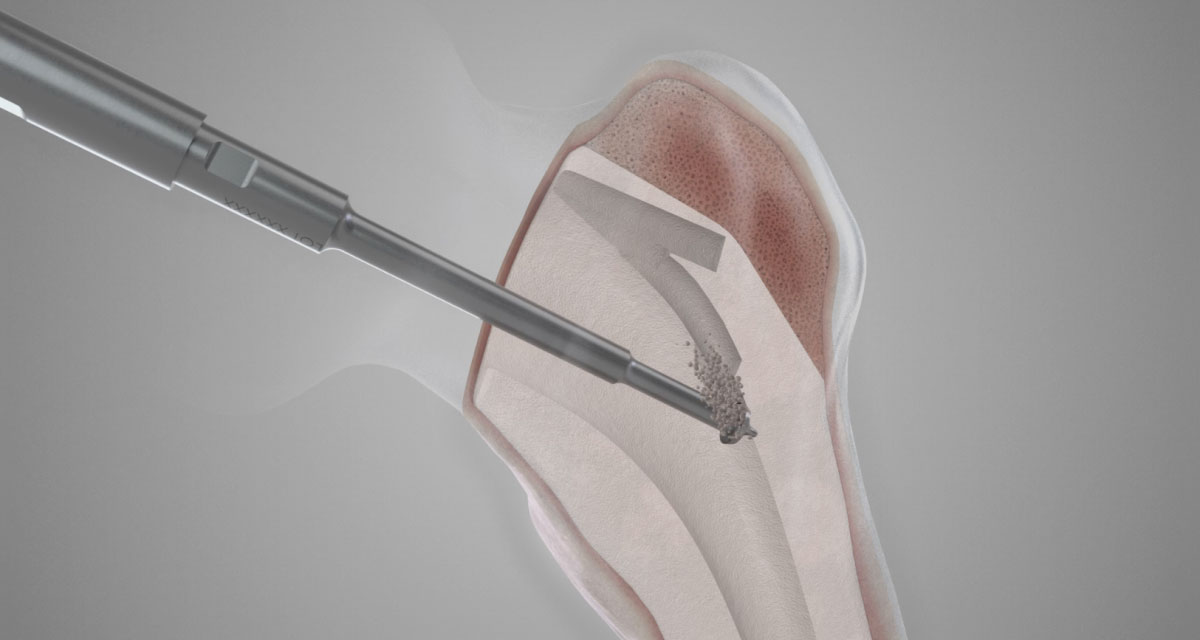
Of these, ultrasonic removal of cement has been demonstrated to be an efficient and safe method to address the challenges posed in an already complex surgical area. These devices use ultrasounds to target cement removal in a safe, predictable, and precise manner. In response to the ultrasonic energy emitted by these devices, the bone cement immediately changes to a putty-like consistency allowing its easy removal while the natural bone remains unaffected. By using specially designed handsets and probes combined with portable ultrasonic generators, ultrasonic devices are a viable option to address the problems associated with revision surgeries.
Mode of Action of Ultrasonic Devices
Bone cement absorbs heat energy caused by the friction at a frequency range of 28.0-30.0kHz. Upon absorbing the heat energy, the physical state of the bone cement changes from a solid to a molten/putty-like consistency, removing it from the bone interface. As a result, the technique reduces the need to use manual force and minimizes the risk of bone fracture and perforation. Another advantage of using ultrasonic devices are the different probe options, the design of which allows for all residual cement to be removed from all the difficult-to-access areas during surgery. The ultrasonic energy waves penetrate beyond the point of contact, extending into the immediately surrounding area of action and allowing more efficient cement removal.
Overall, ultrasonic devices are a viable alternative to address the key challenges of cement removal in revision arthroplasty and hold the potential to improve overall prognosis of the replacement procedure and, eventually, improve the overall quality of life of the patient.
References
- M. Tovar-Bazaga, D. Sáez-Martínez, Á. Auñón, F. López-Oliva, B. Pardos-Mayo, and E. Calvo, “Surgical Technique of a Cement-On-Cement Removal System for Hip and Knee Arthroplasty Revision Surgery,” Arthroplast. Today, vol. 9, 2021, doi: 10.1016/j.artd.2021.05.008.