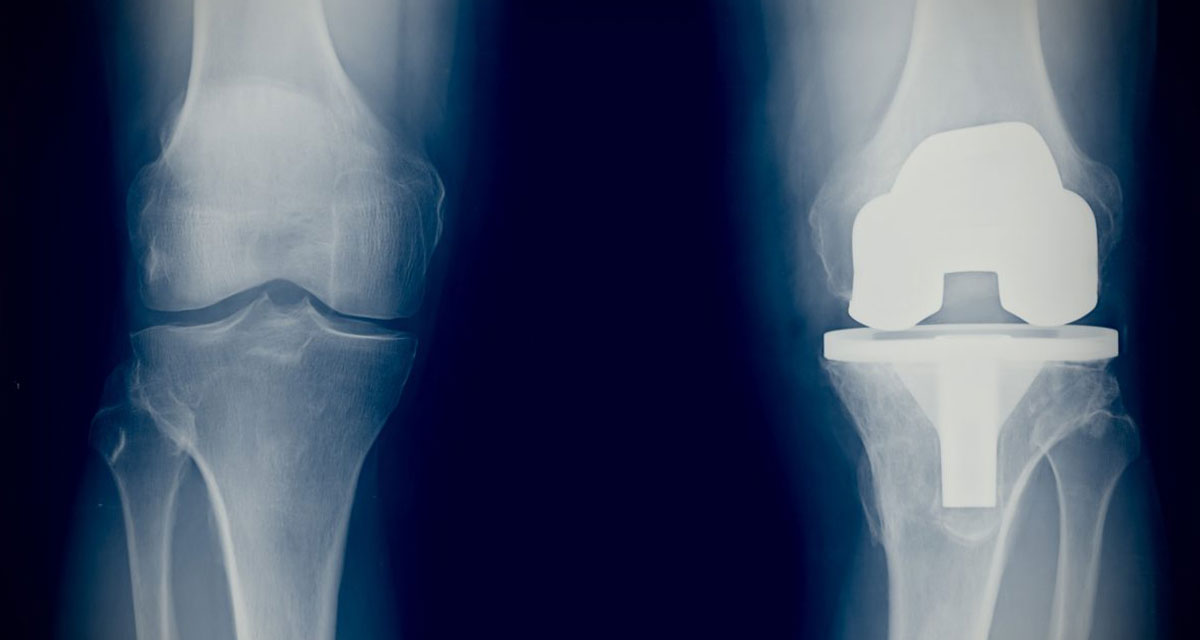
Painful arthritic and inflammatory conditions of the joints are common and often lead to the need for surgical intervention. Severe cases require complete joint replacement such as total knee arthroplasty, total hip replacement and total shoulder or elbow arthroplasty.
Total knee arthroplasty (TKA) is one of the most cost-effective and consistently successful surgeries performed in orthopedics. It provides reliable outcomes for patients suffering from end-stage, tri-compartmental, degenerative osteoarthritis (OA). While OA affects millions of Americans, the knee is the most commonly affected joint plagued by this progressive condition which is hallmarked by a gradual degeneration and loss of articular cartilage.[1]
Total hip arthroplasty (THA) is also a highly successful and cost-effective intervention for addressing pain and functional deficits in patients with advanced hip disease. Although the results of THA are generally excellent, some prostheses eventually fail. In many such cases, revision surgery is performed. In the US, over 50,000 revision THAs are performed every year at a direct cost exceeding $1 billion. Due in part to continued growth in the utilization of primary THA, the number of revisions may increase substantially in the coming decades.[2]
When it comes to upper limbs, shoulder arthroplasty is a prevalent joint replacement surgery, being the third most common after hip and knee replacement. The most common etiology for primary surgery in North America and Europe is osteoarthritis or glenoid arthrosis (38%). The most common revision indication overall is rotator cuff tear, deficiency, or arthropathy (26%).[3]
Lastly, total elbow arthroplasty has higher complication rates compared with arthroplasty procedures for other joints. With new anti-rheumatic treatments, the population receiving total elbow arthroplasty has shifted from patients with rheumatoid arthritis to those with post-traumatic arthritis, further compounding the high complication rate. Common failure mechanisms that often lead to revision include infection, aseptic loosening, fracture, component failure, and instability.[4]
Revision Arthroplasty
After a total joint replacement has been performed, a revision procedure may be necessary over time, when an existing old or worn-out hip, knee, shoulder, or elbow component needs to be removed and replaced with a new or improved prosthesis.
Revisions are modifications or replacements made to an existing artificial joint prosthesis/component.
The principles of revision arthroplasty are to understand the cause of failure, adequate surgical exposure, restoration of limb alignment, achieving appropriate soft tissue balance, correct implant alignment, restoration of joint line and a good range of motion.
Causes of revision arthroplasty include:
- Implant wear and loosening
- Infection
- Recurrent dislocation
- Fracture
- Instability
- Stiffness
- Reaction to metal ions/metal allergy
Due to the deteriorating condition of the prosthesis, the challenges involved to achieve a successful revision arthroplasty procedure include:
- difficulty in appropriate visualization of the surgical area
- ambiguity in discriminating between cement and bone
- unpredictable scheduling that can result in unnecessary complications.
To address these challenges, ultrasonically powered surgical systems are a viable treatment option. Ultrasound is currently the most effective and safe energy form available for powering surgical instruments. Using a series of specially designed handsets and probes combined with portable ultrasonic generators, these devices use ultrasound to target cement removal in a safe, predictable, and precise manner. Bone cement immediately responds to ultrasonic energy and changes to a putty-like consistency allowing its easy removal. The key factor is that the natural bone remains unaffected by this procedure.
The possible risks and complications of revision surgery include:
- Poor wound healing
- Reduced range of motion or stiffness in the knee
- Infection in the wound or the new prosthesis
- Bleeding
- Blood clots in the legs, which may travel to the lungs (pulmonary embolism)
- Bone fracture during surgery
- Damage to nerves or blood vessels
- Medical problems such as heart attack, lung complications, or stroke
Nonetheless, most patients who have revision surgery experience favorable long-term outcomes, including relief from pain and increased stability and function. Although complete pain relief and restoration of function is not always achievable, the low force cutting combined with precise energy dispersion to the surgical site demonstrates that ultrasonically powered osteotomes will address the current challenges to revision arthroplasty procedures, making ultrasonic powered revision arthroplasty one of the most effective options available for revision cases.
References
- M. Varacallo and N. A. Johanson, Total Knee Arthroplasty (TKA) Techniques. 2018.
- J. J. Prokopetz, E. Losina, R. L. Bliss, J. Wright, J. A. Baron, and J. N. Katz, “Risk factors for revision of primary total hip arthroplasty: A systematic review,” BMC Musculoskeletal Disorders, vol. 13. 2012. doi: 10.1186/1471-2474-13-251.
- G. S. A. Nikolas K Knowles 1, Melanie P Columbus 2, Kilian Wegmann 3, Louis M Ferreira 1, “Revision shoulder arthroplasty: a systematic review and comparison of North American vs. European outcomes and complications,” J Shoulder Elb. Surg, vol. May;29(5):, 2020.
- M. A. Ramirez, E. V. Cheung, and A. M. Murthi, “Revision total elbow arthroplasty,” Journal of the American Academy of Orthopaedic Surgeons, vol. 25, no. 8. 2017. doi: 10.5435/JAAOS-D-15-00479.